Being told you have IBD can be an incredibly stressful time. But there are clear benefits when newly diagnosed patients are well informed about their condition and how it can be treated. Not only are they in a better position to adapt to the physical, social and psychological impact of IBD, but they also show improved ability and confidence to manage their condition.
Case study: New diagnosis clinic, St Mark’s Hospital
Statement 1.10
In their clinical encounters, patients should receive personalised signposting to easily accessible information about IBD, the local IBD service and patient organisations in a variety of formats that meet all needs.
Statement 3.3
Patients should be supported to make informed, shared decisions about their treatment and care to ensure these take their preferences and goals fully into account.
Statement 7.2
Patients should be supported in self-management, as appropriate, through referral or personalised signposting to education, groups and support.
Who's doing it well?
In a survey of 150 patients at St Mark’s Hospital, London, 60% of patients perceived themselves to be well-informed about their condition yet reported low levels of knowledge on self-management during a flare. 80% expressed a wish for more information on how to manage their IBD. There was no framework to offer regular education to support shared decision making early in the disease course.
The idea
The Inflammatory Bowel Disease (IBD) team at St. Mark’s Hospital based at London North West University Healthcare Trust set up a dedicated new IBD diagnosis clinic as part of a service improvement project.
This clinic offers 45 minutes for each patient and is run by an IBD physician and an IBD Nurse Specialist. Patients are provided with information on self-management, surveillance of their disease activity, and reliable sources of information (Crohn’s & Colitis UK, and the St Mark’s Flare Management Card and Service Information booklet).
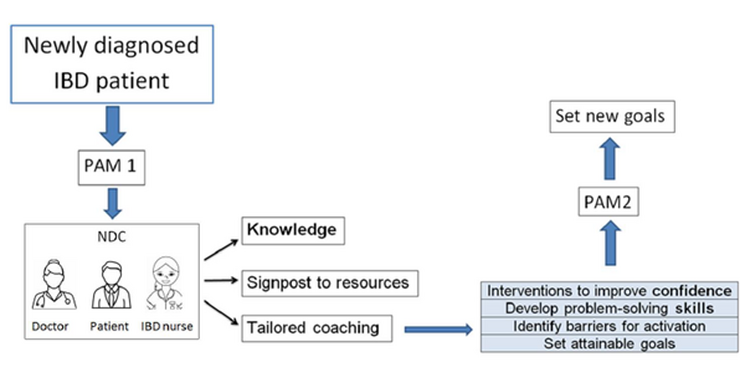
Results
The effectiveness of this service has been objectively assessed using the Patient Activation Measure (PAM) tool. Patient activation was measured before and after the first consultation. PAM is a validated questionnaire that measures knowledge, skills and confidence in patients and captures the extent to which people feel engaged and confident in taking care of their condition. Anxiety and depression were also assessed using the Generalised Anxiety Disorder scale and Patient Health Questionnaire at the first clinic visit.
The PAM showed that half of the patients attending the clinic had low levels of activation before the first consultation. With tailored education, 57% had an improved PAM score. Depression was also found to be a potential barrier to patient empowerment. Early assessment of patients’ activation levels and mental health was recommended to guide healthcare providers to offer individualised care.
The team are currently assessing if this level of improvement was maintained after 6 months and 12 months following their clinic attendance.
I really enjoy working in the IBD New Diagnosis clinic. As a healthcare professional, I have found the clinic to be hugely rewarding. Having the time to go through the patients’ concerns and questions in a protected time slot is very useful for both the patient and for me. The clinic helps to stabilise the foundations of a good patient and clinician relationship. The COVID-19 pandemic has created some obstacles. We have managed to navigate some of these by introducing the virtual video platform “Attend Anywhere”. Feedback has been positive overall, however, there is a keen want to get back to face-to-face reviews from both the healthcare professional and patients. I have also learnt a lot from my MDT physician, and I would like to think they have learnt something from me!
Date created: April 2021